-
 Sanjay Kokate 1 week ago
Sanjay Kokate 1 week agoThe Evolving Landscape of Cervical Cancer Treatment
As we move deeper into 2025, the treatment options for cervical cancer continue to evolve at an unprecedented pace. I've been following these developments closely, and I'm excited to share how immunotherapy is revolutionizing treatment approaches. You may have noticed the shift from conventional therapies toward more personalized, immune-based strategies. This transformation represents a significant leap forward in how we address this challenging disease.
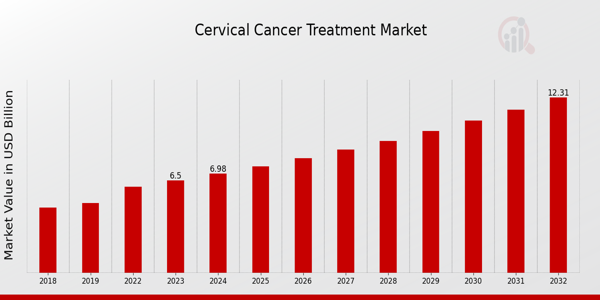
The latest statistics show cervical cancer remains a significant health concern worldwide. Yet the emergence of novel immunotherapy approaches offers renewed hope. These treatments harness the body's natural defenses. They teach immune cells to recognize and attack cancer. The results have been remarkable in many cases.
Immunotherapy: The New Frontier in Cervical Cancer Management
Immunotherapy has emerged as the cornerstone of modern cervical cancer treatment. You might wonder how it differs from traditional approaches. Unlike chemotherapy that attacks all rapidly dividing cells, immunotherapy works selectively. It targets cancer cells specifically. This means fewer side effects for your patients.
Several immunotherapy types now show promise:
- Immune checkpoint inhibitors that remove the "brakes" cancer places on immune responses
- Therapeutic vaccines that stimulate immune recognition of HPV-infected cells
- Adoptive T-cell therapies using the patient's enhanced immune cells
- Combination approaches that pair immunotherapy with traditional treatments
- Personalized neoantigen vaccines tailored to individual tumor mutations
The precision of these approaches allows for treatment customization. You can now match therapy to specific patient profiles. This personalization significantly improves outcomes. It reduces unnecessary treatments and side effects.
Integration of AI in Treatment Planning and Monitoring
Artificial intelligence now plays a crucial role in cervical cancer management. You likely have already encountered some AI tools in your practice. These systems analyze vast datasets quickly. They identify patterns humans might miss. They predict treatment responses with remarkable accuracy.
AI algorithms now help optimize immunotherapy protocols. They can predict which patients will respond best. They monitor treatment effectiveness in real-time. They even suggest modifications based on emerging biomarkers.
The integration of AI with imaging has transformed monitoring. You can track treatment response with unprecedented precision. Subtle changes that might indicate resistance appear early. This allows for timely intervention and treatment adjustment.
Biomarker-Driven Treatment Selection
The identification of reliable biomarkers has revolutionized treatment selection. You now have tools to predict immunotherapy response. This capability transforms the clinical decision-making process. It ensures patients receive optimal treatment from the start.
Several biomarker categories guide treatment decisions:
Biomarker Type Clinical Application Impact on Treatment Selection PD-L1 Expression Predicts response to checkpoint inhibitors High expression suggests good immunotherapy response Tumor Mutational Burden Indicates neoantigen presence Higher burden correlates with better immunotherapy outcomes Microsatellite Instability Reflects DNA repair deficiency MSI-High tumors respond well to immunotherapy Immune Cell Infiltration Shows immune recognition Highly infiltrated tumors often respond better HPV Integration Status Indicates viral oncogene activity Affects selection of HPV-targeted therapies Your ability to interpret these biomarkers transforms care delivery. It allows for truly personalized treatment approaches. It maximizes efficacy while minimizing unnecessary treatments.
Novel Combination Therapies Showing Promise
Combination therapy approaches have yielded impressive results. You might find these multimodal strategies particularly effective for advanced cases. They target cancer through complementary mechanisms. They overcome resistance pathways. They produce synergistic effects that improve outcomes.
Current research focuses on several promising combinations. Immunotherapy paired with targeted radiotherapy shows synergy. Adding epigenetic modifiers improves immune recognition. Combining different immunotherapy classes enhances response. These approaches address the multifaceted nature of cervical cancer.
The sequencing of these combination therapies matters greatly. You'll want to consider optimal timing for each component. Some combinations work best concurrently. Others require sequential administration. Careful planning maximizes therapeutic benefit.
Addressing Treatment Resistance Mechanisms
Despite impressive advances, treatment resistance remains challenging. You've likely encountered patients who initially respond well but later relapse. Understanding resistance mechanisms has become crucial. It allows for proactive intervention. It informs second-line treatment selection.
Several mechanisms drive immunotherapy resistance in cervical cancer. Tumor microenvironment changes can suppress immune function. Cancer cells may lose antigens recognized by immune cells. Immune checkpoint molecules may be upregulated. Metabolic pathways may shift to evade detection.
New approaches specifically target these resistance mechanisms. You now have options when first-line treatments fail. These include alternative checkpoint pathways. They include metabolic modulators. They include microbiome-targeted interventions. Each addresses specific resistance mechanisms.
Future Directions and Emerging Technologies
Looking ahead, several technologies promise to further transform treatment. You should watch developments in these areas closely. They represent the next wave of innovation. They may soon become standard components of care.
Liquid biopsy technologies allow non-invasive monitoring. They detect circulating tumor DNA. They identify emerging resistance early. They guide timely treatment adjustments. They spare patients repeated invasive procedures.
Nanotechnology delivery systems improve therapeutic targeting. They deliver immunotherapy agents directly to tumors. They reduce systemic exposure. They enhance efficacy while minimizing toxicity. They overcome biological barriers to treatment.
Implementing Advanced Treatments in Clinical Practice
Transitioning these advanced treatments to clinical practice presents challenges. You may face implementation barriers in your setting. These might include cost concerns. They might include technical requirements. They might include training needs.
Multidisciplinary collaboration becomes essential. You'll need to work closely with various specialists. These include pathologists for biomarker testing. They include data scientists for AI implementation. They include pharmacists for complex regimen management.
Patient selection remains critical for success. You must carefully assess eligibility criteria. You must consider comorbidities and performance status. You must evaluate prior treatment history and response. Thorough assessment ensures optimal outcomes.
Conclusion
The cervical cancer treatment landscape continues to evolve rapidly. Immunotherapy has established itself as a transformative approach. You now have unprecedented tools to personalize treatment. You can predict responses. You can monitor outcomes. You can adapt strategies based on emerging data.
As these innovations continue to mature, your role as a healthcare professional becomes increasingly important. Your understanding of these complex therapies guides implementation. Your expertise ensures patients receive optimal care. Your insights drive further innovation.
The future of cervical cancer treatment looks increasingly promising. Continued research and clinical experience will refine these approaches. They will enhance efficacy. They will minimize toxicity. They will improve quality of life. Together, we're reshaping the future of cervical cancer care.
-
 Rank Xone 1 week ago
Rank Xone 1 week agodeep tissue massage is perfect for relieving sore muscles. It might feel intense, but the results are totally worth it!